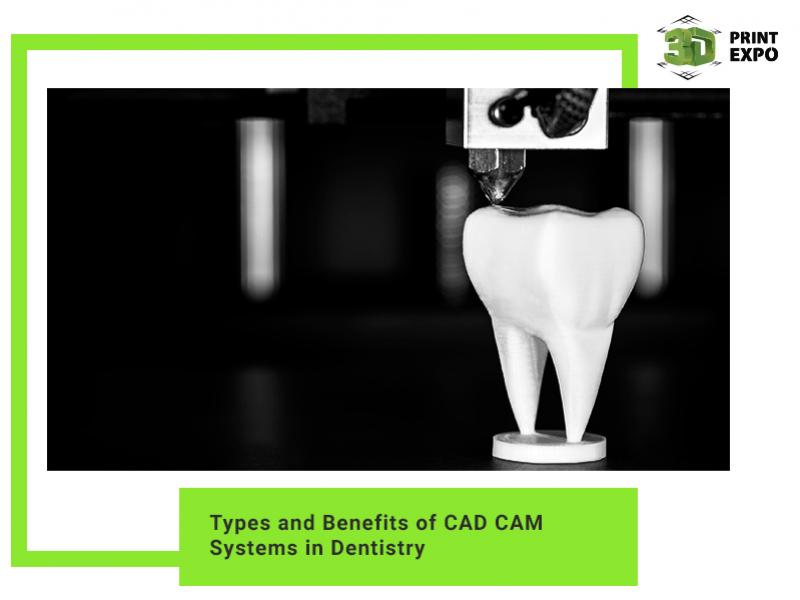
Trachea 3D Printed with Ordinary MakerBot PLA
We may await the day that 3D bioprinting is ubiquitous practice, but MakerBot and The Feinstein Institute for Medical Research have proven that we may not have to wait that long. Using ordinary MakerBot PLA filament, the Feinstein researchers were able to create custom scaffolding on which living cells were cultured for a tracheal implant. The results of the research were presented at the the 51st Annual Meeting of The Society of Thoracic Surgeons in San Diego by Feinstein investigator Todd Goldstein.
Repairing narrow or weak trachea – resulting from cancer, intubation, and blunt trauma, among other possibilities – is typically a difficult process, with the two most popular techniques suffering from limitations. For this reason, Drs. Lee Smith and David Zeltsman, of the North Shore-LIJ Health System, began considering the process 3D printing and engineering tissue for tracheal repair, believing that such technology was still ten to twenty years in the making. The two then turned to Goldstein, a PhD candidate at the Hofstra North Shore-LIJ School of Medicine, and Daniel A. Grande, director of the Orthopedic Research Laboratory at the Feinstein Institute, who spent the past year examining the possibility of repairing and replacing damaged trachea using 3D printing and tissue engineering. And, in just one month, Goldstein and Grande were able to pull of the 3D printing and engineering of a human trachea.

The Feinstein Institute had previously been able to culture cartilage by binding chondrocytes and growth nutrients via collagen, but had yet to construct that cartilage into a useful structure. By 3D printing the scaffolding from PLA on a MakerBot Replicator 2X Experimental 3D Printer, however, the researchers were able to make a significant breakthrough. Goldstein explains, “Making a windpipe or trachea is uncharted territory. It has to be rigid enough to withstand coughs, sneezes and other shifts in pressure, yet flexible enough to allow the neck to move freely. With 3D printing, we were able to construct 3D-printed scaffolding that the surgeons could immediately examine and then we could work together in real time to modify the designs.”
Existing bioprinters can have pricetags that range in the tens to hundreds of thousands of dollars, a sum that Feinstein refused to spend. The desktop 3D printers on which most bioprinting technology is currently based, however, can cost below the $1,000 mark. Goldstein opted for modifying this low-cost technology for his own bioprinting needs, relying on the help of MakerBot along the way.
The mods for Feinstein’s bioprinter can be found on Thingiverse: Nick’s Universal Paste Extruder Derivative by nicksears, Print PLA with MakerBot Replicator 2X Upgrade by 3dprintler, Threaded Filament Dust Filter – Replicator 1,2 & 2X by ppyromann
Goldstein says, “MakerBot was extremely helpful and consulted on optimizing our design files so they would print better and provided advice on how to modify the MakerBot Replicator 2X Experimental 3D Printer to print with PLA and the biomaterial. We actually found designs to modify the printer on MakerBot’s Thingiverse website to print PLA with one extruder and the biomaterial with the other extruder. We 3D printed the needed parts with our other MakerBot Replicator Desktop 3D Printer, and used them to modify the MakerBot Replicator 2X Experimental 3D Printer so that we could better iterate and test our ideas.”

After tackling the hurdle of getting his hands on a bioprinter, Goldstein had to determine what sort of material would be useable in a surgical scenario. He then realized that ordinary PLA could be made sterile as it was heated by the printer’s hotend, with Dr. Smith saying, “The advantage of PLA is that it’s used in all kinds of surgical implant devices.” Out of the second extruder, the printer lays the Feinstein’s cartilage creating bio-ink. The ink fills in the gaps in the PLA scaffolding before curing into a gel on the printer’s heated build plate.
The resulting print, a two-inch-long tubular piece of trachea, is then placed into a bioreactor. Such devices, which ensure even growth and adequate temperature for the living cells, can cost between $50,000 and $150,000. Again, Goldstein turned to his desktop 3D printer, creating the gears and other components for his own, custom incubator. Dr. Smith adds, “The ability to prototype, examine, touch, feel and then redesign within minutes, within hours, allows for the creation of this type of technology. If we had to send out these designs to a commercial printer far away and get the designs back several weeks later, we’d never be where we are today.”

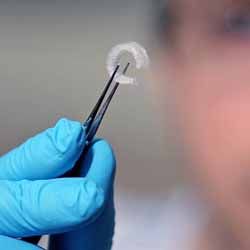
Surviving four weeks in the incubator, the trachea is a proof-of-concept for what could be. The abstract for Goldstein’s study explains how the trachea cartilage was able to grow similar to that of an actual windpipe, “The cells survived the 3D printing process, were able to continue dividing, and produced the extracellular matrix expected of tracheal chondrocytes.” The next stage is much continued research and FDA approval.
Dr. Smith believes that day might be just five years away. Saying that the North Shore-LIJ Health System sees at least one patient a year that cannot be helped by the two prevailing tracheal repair techniques. In the future, though, he believes that it might be possible to harvest a patient’s own cells and grow them on custom, 3D printed scaffolding. This approach would be particularly advantageous for helping children. Smith says, “There’s really a limitless number of sizes and permutations you might need to reconstruct an airway in a child.”

He continues, “This project will probably define my scientific career. As we produce something that can replace a segment of trachea, we’ll constantly be modifying and optimizing, the correct bio materials, the correct way to bond the cells to the scaffold. 3D printing and tissue engineering has the potential to replace lots of different parts of the human body. The potential for creating replacement parts is almost limitless.”
Goldstein, now Feinstein’s resident 3D printing specialist, believes that his course has been guided by the research, saying, “Knowing that I can make a part that will save someone’s child — that’s life-changing.”
MakerBot is continuing to support the staff at Feinstein, providing their new composite PLAs to the institute for the researchers to explore the possibilities of calcium carbonate and iron filaments. Jenny Lawton, CEO of MakerBot, contributed, “The research being done at the Feinstein Institute is exciting and promising. We are continually amazed by what is being created with 3D Printers. To know that a MakerBot Replicator 3D Printer played a role in a potential medical breakthrough is inspiring.”
Dr. Grande, who originally turned to the Feinstein researchers for the project, puts a nice concluding touch on the story, saying, “Do you remember the Six Million Dollar Man? The Bionic Man is not the future, it’s the present. We have that ability to do that now. It’s really exciting.”
For a more technical telling of the story, watch the Feinstein video below: